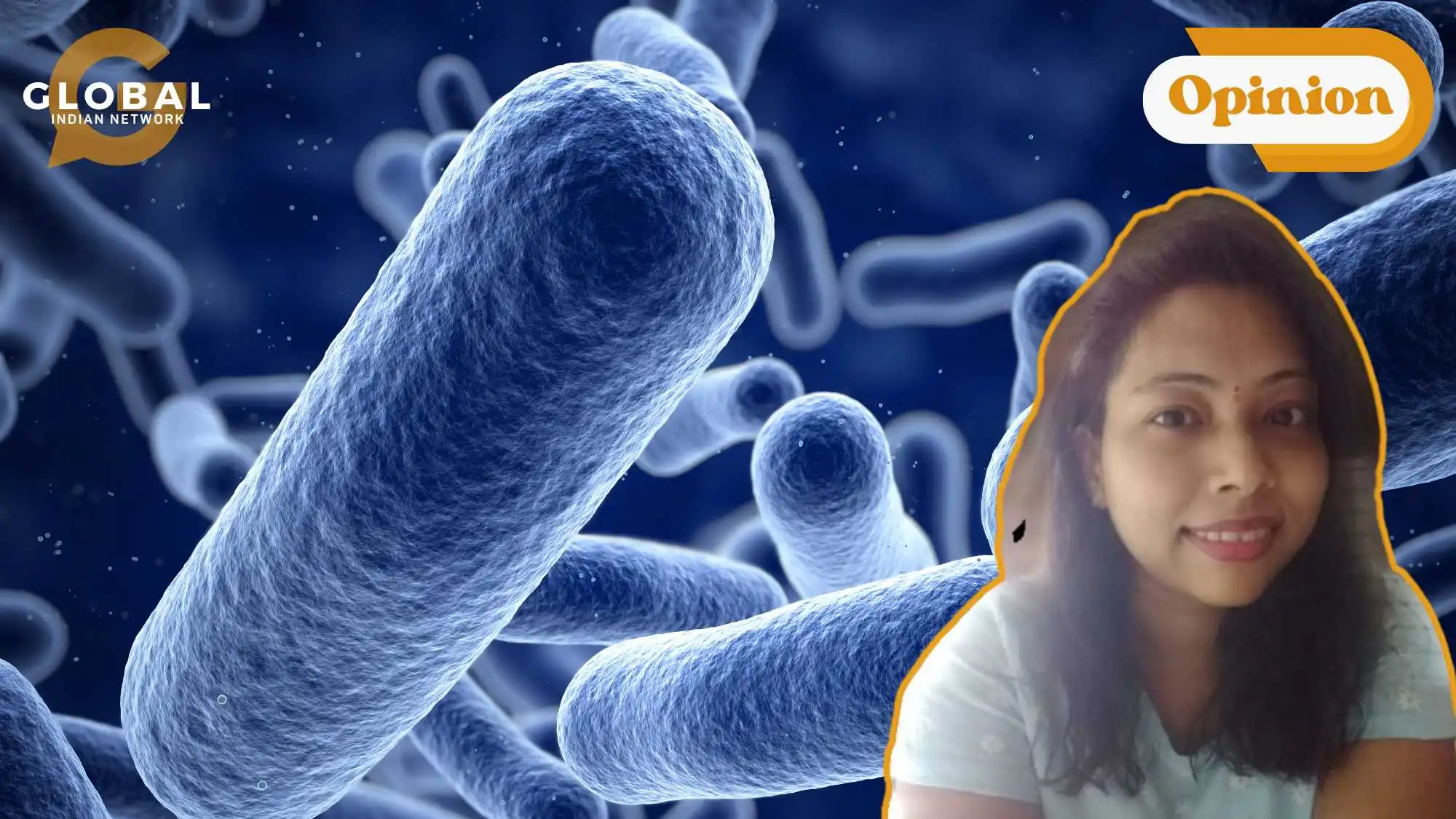
Can flu kill you in two days? This ain’t a silly question. Sorry to tell you, yes it does! An infection that eats up tissue like a flesh-eating monster. That’s the terrifying reality in Japan right now.
A bacterial infection called Streptococcal Toxic Shock Syndrome (STSS) is on the rise. This infection can be deadly and turns serious very quickly. Let’s see what’s going on and how to remain safe.
Japan is currently experiencing a surge in cases of Streptococcal Toxic Shock Syndrome (STSS), a bacterial infection caused by Group A Streptococcus (GAS) bacteria.
The National Institute of Infectious Diseases, Japan, released an official statement in March 2024 about its increasing rates.
As of June 2, 2024, there have been 977 reported cases, greater than the previous record of 941 cases in all of 2023.
STSS is also known as “flesh-eating bacteria”, as it leads to rapid tissue destruction and organ failure if left untreated.
The disease has a mortality rate of up to 30% and has claimed 77 lives in Japan between January and March 2024.
Group A Streptococcus. Source: NIAID
Symptoms
Let’s look at the symptoms
- Fever and chills
- Muscle aches
- Nausea and vomiting
- Low blood pressure (hypotension)
- Rapid heart rate (tachycardia)
- Rapid breathing (tachypnea)
- Rash resembling sunburn
- Organ failure (e.g. kidney, liver, lungs)
- Confusion or disorientation
Source: https://www.cdc.gov/group-a-strep/about/cellulitis.html
How Quickly Can STSS Progress?
STSS can progress quickly within 24-48 hours, from the initial flu-like symptoms to more severe complications like organ failure and shock.
Ken Kikuchi, a professor in infectious diseases at Tokyo Women’s Medical University stated that “most of the deaths happen within 48 hours” of patients noticing the initial symptoms.
The rapid progression of STSS is a major concern, as the disease.
According to the U.S. Centers For Disease Control & Prevention, immediate medical attention is important, as STSS can be fatal in up to 30-40% of cases.
Differentiating STSS from Staphylococcal Toxic Shock Syndrome (TSS)
STSS is almost always associated with an invasive group A Streptococcus (GAS) infection, while Staphylococcal TSS is often associated with localized infections like pneumonia, osteomyelitis, or skin wounds.
Patients with Staphylococcal toxic shock syndrome (TSS) often develop a red, flat rash that peels whereas, patients with Streptococcal Toxic Shock Syndrome (STSS) tend to have a widespread red rash that turns white when pressed.
In 60-80% of Streptococcal toxic shock syndrome (STSS) cases, blood tests show the presence of bacteria but only about 3% of Staphylococcal toxic shock syndrome (TSS) cases show bacteria in blood tests.
Diagnosing STSS
The diagnosis of STSS requires hypotension, multi-organ involvement, and isolation of GAS bacteria.
However, these diagnostic criteria have poor sensitivity early in the disease course, when patients may only present with fever and rash without meeting the full criteria.
Therefore, the absence of meeting the formal diagnostic criteria should not delay early diagnosis and treatment of suspected STSS.
Preventive Measures
Prompt treatment of any Streptococcal infections, such as strep throat or skin infections, is crucial to prevent progression to STSS.
Maintaining good hygiene practices, including regular handwashing and covering coughs/sneezes.
Proper wound care, such as immediate cleaning and dressing of cuts, scrapes, or surgical sites.
Public health measures like monitoring and education campaigns can help raise awareness about STSS symptoms.
Treatment
STSS is a medical emergency requiring immediate hospitalization and treatment.
The main treatment includes giving high-dose intravenous antibiotics, usually a combination of Penicillin and Clindamycin.
Fluid balance, medications to maintain blood pressure, and potential organ support (e.g. dialysis, mechanical ventilation).
In severe cases of deep tissue infections, removal of infected tissue may be necessary.
LISTEN TO THIS PODCAST: Exploring Immigrant Identity and Trailing Spouses in Japan with Dr Megha Wadhwa
Final Words
The exact reason for the outbreak is unclear, but experts suggest that the relaxation of COVID-19 measures has led to a rise in respiratory infections, which may have weakened people’s immune systems during the pandemic.
The fight against STSS in Japan is a race against time. With exponentially increasing cases, early diagnosis and treatment are important. Let’s hope Japan will turn the tide of the situation and emerge victorious. Do you think this disease has a scope to become the next pandemic? Let us know in the comments below.
Do you have burning thoughts or opinions? We’d love to hear them! Feel free to reach out to us at larra@globalindiannetwork.com